The Medicare trust fund finances health services for beneficiaries of Medicare, a government insurance program for the elderly, the disabled, and people with qualifying health conditions specified by Congress. The trust fund is financed by payroll taxes, multiple general revenue sources, and the premiums enrollees pay.
The Medicare trust fund comprises two separate funds. The hospital insurance trust fund is financed mainly through payroll taxes on earnings and income taxes on Social Security benefits. The Supplemental Medical Insurance trust fund is financed by general revenues and the premiums enrollees pay. Taken together, total Medicare costs have risen from just above 2 percent of GDP in 2000 to 4 percent in 2020 and projected by the Center for Medicare and Medicaid Services or CMS to rise to 6 percent by 2047. Under an “illustrative alternative” estimated by the CMS actuaries, those costs might rise to 8 percent of GDP by 2040. They are financed by a complex web of 15 different streams, including several forms of general revenue transfers, including the borrowing or federal deficits that are a part of general revenues (Steuerle 2023).
Hospital Insurance Trust Fund
The hospital insurance (HI) trust fund, also known as Part A of Medicare, finances health care services related to hospital stays, skilled nursing facilities, and hospices for eligible beneficiaries—mainly Social Security recipients over age 65 or receiving Social Security Disability Insurance.
The HI trust fund had revenue of $387 billion and a balance of $178 billion at the end of 2022 (table 1). The fund’s chief revenue sources are payroll taxes, income from the taxation of Social Security benefits, and income from a 3.8 percent surtax on investment income of high-income individuals. Interest payments on trust fund balances, premiums from voluntary enrollees ineligible for Medicare coverage based on their earnings records, transfers from the general fund and the Railroad Retirement account, and miscellaneous receipts supply the remainder of revenues.

Supplemental Medical Insurance Trust Fund
The Supplemental Medical Insurance (SMI) trust fund finances two voluntary Medicare programs: Part B, which mainly covers physician services and medical supplies, and Part D, the newer prescription drug program.
The combined SMI trust fund received $571billion in income and had $171billion in assets at the end of 2022 (table 2). Unlike the HI fund, no payroll taxes are dedicated to SMI. Instead, almost all the fund’s income comes from contributions from the general fund (receipts from other sources, such as individual income taxes, corporate taxes, excise taxes, and borrowing) and premiums from participants (there are separate premiums for Parts B and D, and a higher set of premiums within each Part for higher-income beneficiaries). Because the bulk of SMI’s funding comes from the general fund, the trust fund balance mainly serves to cover temporary shortfalls and is kept low. High reserves are not required as long as general fund revenues and borrowing automatically rises with costs.

Solvency and Budget Pressures
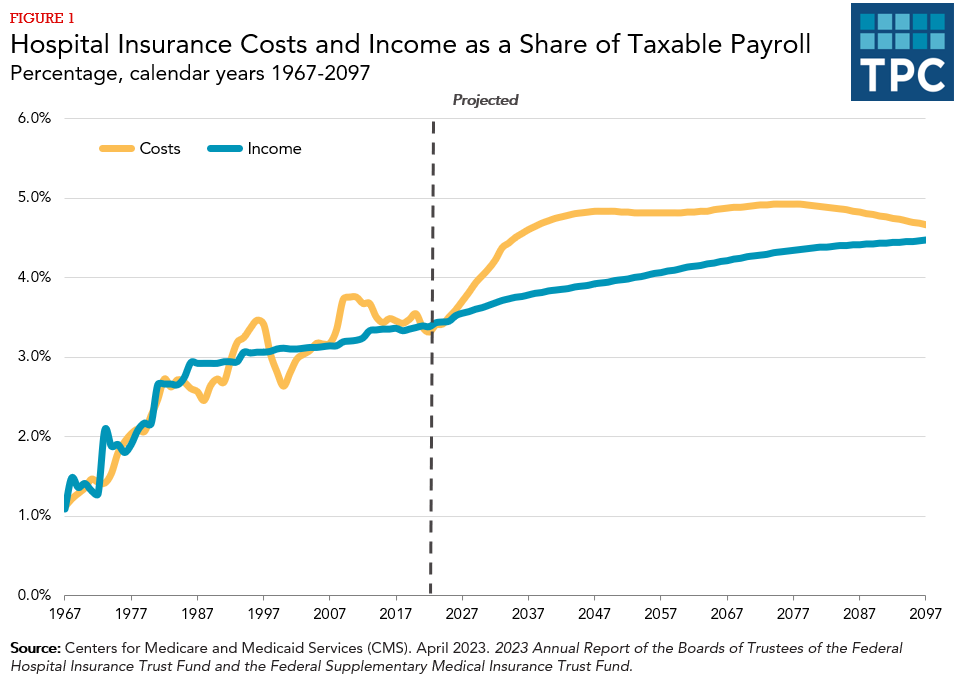
Like the Old-Age and Survivors Insurance and Disability Insurance trust funds, the HI trust fund faces long-term deficits (figure 1). (The SMI fund, primarily financed by general revenue, does not face these trust fund imbalances, though it still adds substantial growingpressure to the overall budget.) While the number of Medicare beneficiaries increased by around 2 percent annually from 2023 to 2032, the decline in the birth rate starting about 1965 now puts much greater pressure on the worker-to-retiree ratio. That ratio was about 4 from 1980 to 2008, declined to 2.9 in 2022, and is estimated to decline further to 2.5 in 2030 and to 2.2 by 2097. Meanwhile, the cost of health care has increased rapidly as well. Though this cost dynamic has slowed but not stopped, the aftermath from the COVID-19 crisis still remains uncertain, and much is dependent upon the direction of future policy.
Updated January 2024
Centers for Medicare and Medicaid Services. 2023. 2023 Annual Report of the Boards of Trustees of the Federal Hospital Insurance and Federal Supplementary Medical Insurance Trust Funds. Baltimore, MD.
Congressional Budget Office. 2022. The 2022 Long-Term Budget Outlook. Washington, DC.
Shatto, John D., and M. Kent Clemens. 2023. “Projected Medicare Expenditures under an Illustrative Scenario with Alternative Payment Updates to Medicare Providers.” Baltimore, MD: Centers for Medicare and Medicaid Services.
Steuerle, C. Eugene and Bowen Garrett. 2022. “The Medicare Financing Conundrum: Revenues, Spending, and Short- and Long-Term Fiscal Challenges.” Washington, DC: The Urban Institute.
Steuerle, C. Eugene. 2023. “Congress’s Medicare Financing Mess is Bigger Than You Think.” TaxVox (blog). Washington, DC: Urban-Brookings Tax Policy Center.